Wisdom Teeth
Do Wisdom Teeth Need Removing? (When to Act and When to Leave Them Alone)

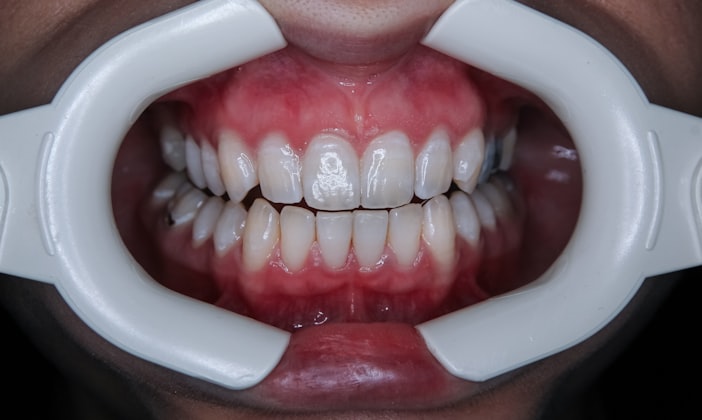
Short, honest answer: it completely depends on what your specific wisdom teeth are doing. There's a real cultural assumption that everyone needs their wisdom teeth out eventually, and it's just not true. About 30% of adults have wisdom teeth that come through fully, sit in the right place, and never cause any trouble at all. Those teeth are as useful as any other molar and there's no reason to touch them. Pulling a perfectly good tooth for no clinical reason is not something any decent dentist is going to recommend.
The other 70% is where it gets more interesting, and that's really where this post lives. Some of those teeth absolutely need to come out, sometimes urgently, and we'll explain the signs that make removal the clear call. Others sit in a greyer zone where it's a genuine judgement call about probability and timing. A smaller group should be actively left alone because removing them would cause more problems than leaving them in.
What decides the answer in any particular case is almost always the X-ray, specifically what it shows about the angle of the tooth, the relationship to the neighbouring molar, how close the roots sit to the main jaw nerve, and whether there's any sign of a problem quietly developing. At UrgentCare Dental, a wisdom tooth assessment with X-ray is £20, and you'll leave with a proper answer, not a hedge.
When the Answer Is Clearly Yes
There's a small number of specific situations where wisdom tooth removal is genuinely the right call, and in those cases the clinical evidence is strong enough that most dentists will make the same recommendation.
Recurrent pericoronitis is the most common one, and if you've had it even twice you'll know exactly why. Pericoronitis is an infection that sets in under the flap of gum that drapes over a partially erupted wisdom tooth. The anatomy itself creates a bacterial trap, so antibiotics clear the current infection but don't change the underlying setup that caused it. Each flare-up is a miserable week of pain and antibiotics and feeling rough, and then a quiet period, and then another flare-up. Once this cycle has happened two or three times, the pattern is established and it's essentially certain to keep happening. Extraction is what ends the cycle, and when patients hear "this problem won't ever come back once the tooth is out," that tends to make the decision pretty quickly.
Damage to the neighbouring molar is the strongest case for preventive removal even when the wisdom tooth itself isn't causing symptoms. When an impacted wisdom tooth pushes forward into the second molar, it can cause decay on the back surface of that molar, in a location that's essentially impossible to clean or fill properly while the wisdom tooth is in the way. The X-ray shows it clearly: the impacted tooth pressed tight against its neighbour, a dark shadow of cavity forming at the contact point. The choice then becomes straightforward, because the second molar is a much more valuable tooth than the wisdom tooth (you actually use it for chewing), and protecting it by removing the wisdom tooth is obviously the right call. Leaving things alone would mean eventually losing both teeth instead of just one.
Significant decay in the wisdom tooth itself usually tips the decision toward extraction rather than filling, for a combination of reasons that feel almost too practical. Wisdom teeth sit so far back that filling them properly is technically quite difficult, and the restoration is hard to maintain with normal brushing even if the filling is done well. On top of that, wisdom teeth aren't doing any useful chewing work in most cases because they don't have an opposing tooth to bite against properly. So the economic and clinical logic is: a tooth that isn't contributing to your chewing function, that's now got decay in an awkward spot, is generally better removed than patched up.
Cyst formation around an impacted wisdom tooth is uncommon but serious enough to warrant immediate attention. The little sac of tissue that surrounds an unerupted tooth can sometimes develop into a fluid-filled cyst that slowly expands into the surrounding jaw bone. These are usually painless and typically discovered by chance on a routine X-ray, but left alone they can compromise significant amounts of bone. Removing both the cyst and the tooth that caused it, early while it's still small, is a much simpler procedure than dealing with a large cyst that's eroded years of bone.
And finally, if you're having or about to have orthodontic treatment, wisdom teeth that might push other teeth out of alignment as they try to erupt often come out as part of protecting the investment you're making in getting your teeth straight. This one's a judgement call and not every ortho case needs wisdom teeth removed, but it's on the list of things to think about if you're planning to straighten your teeth.
When the Answer Is Clearly No
Just as clearly, there are situations where wisdom teeth should be left alone, and a dentist who recommends removal in these cases is either misreading the X-ray or, honestly, not giving you good advice. Worth knowing about them so you can push back if needed.
If your wisdom teeth are fully erupted, well-positioned, and symptom-free, and they're actually functioning as part of your dental arch with an opposing tooth to bite against, those are teeth worth keeping. They contribute to your chewing, they're not causing any trouble, and removing a healthy functional tooth for no reason is unnecessary surgery. "You're in your thirties, you should probably get them out" is not a clinical reason. The actual presence or absence of a problem is what matters, not age or general paranoia about wisdom teeth.
Deeply impacted teeth that are showing no symptoms and no signs of pathology can often be monitored indefinitely rather than removed. A wisdom tooth that's buried deep in the bone, oriented vertically, not pressing on anything, and showing no signs of cyst formation or decay may well sit there quietly for your entire life. The watchful approach here is: an X-ray every couple of years to confirm nothing is changing, and as long as the picture stays stable, nothing needs doing. A lot of people in their seventies and eighties still have their wisdom teeth buried in the bone, completely unnoticed, and have never had a problem with them.
Certain medical situations can also tip the balance toward leaving the teeth alone. If you're on blood thinners, bisphosphonates, or other medications that make dental surgery higher-risk, or if you have medical conditions that complicate healing, or if you're older and the surgical risks outweigh the modest benefit of preventive removal, the sensible choice is usually monitoring rather than extraction. A good dentist will weigh all of this as part of the conversation.
Lastly, there are cases where the tooth sits too close to the main nerve in the lower jaw (the inferior alveolar nerve) for safe extraction without specialist techniques. In some patients, the roots of lower wisdom teeth literally wrap around or sit directly adjacent to this nerve. A standard extraction in that scenario carries a real risk of causing nerve damage, which can result in temporary or occasionally permanent numbness of the lower lip and chin. If the X-ray shows this kind of nerve proximity and the tooth isn't currently causing problems, monitoring is often the better path than taking on that risk unnecessarily. If the tooth does need to come out eventually, referral to an oral surgeon with specific experience in nerve-adjacent extractions is how it gets done safely.
The Grey Zone (Where Most Decisions Actually Live)
The honest truth is that most wisdom tooth decisions don't sit at either extreme. They sit in the middle, where the tooth isn't actively causing problems right now but might in the future, and the real question becomes one of probability and timing rather than certainty. This is the conversation that actually matters for most people.
The angle the tooth is sitting at is the biggest single factor here. Mesioangular impactions (where the tooth is tilted forward toward the molar in front of it) are by some margin the most likely to cause future problems, because the angle itself creates pressure on the neighbouring tooth and makes pericoronitis more probable. Vertical impactions (the tooth pointing straight up or down, just buried deep) are much less likely to cause issues if they're not currently symptomatic. Horizontal impactions (lying on their side) are somewhere in between and depend heavily on what they're pressing against. The angle is something you can actually see on the X-ray, and any decent dentist will show you and explain what it means for your specific tooth.
Age is another significant factor, and it genuinely changes the calculation. Younger patients, late teens to mid-twenties, have softer bone, less developed roots, and faster healing. Extracting a wisdom tooth at 19 is a simpler procedure with easier recovery than extracting the same tooth at 45. The roots are shorter, the bone is more forgiving, and you bounce back in a week rather than two. This is one argument for earlier intervention when the probability of future problems is moderate to high: you'd rather have it done when your body handles it well than wait until it becomes more difficult. It's not a reason to extract asymptomatic teeth in someone who'd be fine leaving them alone, but it's a real factor when the decision is already on the table.
Root development matters too. A wisdom tooth with incomplete root formation is easier to remove cleanly and has lower risk of nerve proximity complications. Once the roots are fully formed, they're longer, often curved, and can sit closer to the nerve canal. If extraction is going to happen at some point, doing it before the roots finish developing is usually simpler surgically.
The gum tissue around the tooth tells you something about the future too. A partially erupted tooth with a persistent flap of gum over part of it is essentially going to develop pericoronitis at some point. The pocket is there, the bacterial trap is set, and it's really a question of when, not if. If you're already seeing signs of recurrent mild soreness or occasional swelling around that area, you're watching the cycle start to establish.
Putting this all together is what the dentist does. A mesioangular impaction in a 22-year-old with root development still incomplete and an already-present gum flap? The case for removal is genuinely strong even without current symptoms. A vertical impaction in a 45-year-old with fully formed roots that are close to the nerve and no sign of any problem? The case for leaving it alone is equally strong. The same X-ray findings in different people at different ages can lead to different recommendations, and that's appropriate rather than inconsistent.
What the Dentist Is Actually Looking At
The conversation about wisdom teeth should always happen with an X-ray on the screen in front of you, because the visual evidence is what turns this from an abstract question into a specific one about specific teeth. If a dentist is recommending extraction (or recommending against it) without showing you the X-ray and walking you through what it shows, that's a conversation worth asking more questions in.
What they'll be pointing at includes the angle of each wisdom tooth: is it straight, tilted forward, tilted backward, lying horizontal? The angle predicts both the likelihood of future problems and how complex the extraction would be if it came to that. They'll show you the relationship between the wisdom tooth and the molar in front of it: is there a visible contact point between them, and can you see a shadow of decay starting at that contact? Contact points are where decay develops, and they're often visible quite early on the X-ray if you know what you're looking for.
They'll show you the depth of the tooth, which affects both the probability of symptoms and the complexity of removing it. A tooth that's half erupted and half under the gum is more likely to cause pericoronitis than one that's fully buried or fully through. And for lower wisdom teeth specifically, they'll look carefully at how close the roots sit to the inferior alveolar nerve canal. If the roots appear to overlap or touch the nerve on the standard X-ray, a 3D CT scan is often used to get a more precise view, which plans the extraction safely if one's going to happen.
Finally, they'll look at the bone around the tooth for any dark shadows that might indicate cyst formation or infection. These findings strengthen the case for removal considerably, because cysts don't resolve on their own and infection sitting silently in the jaw isn't something you want to leave indefinitely.
This X-ray conversation is where "do my wisdom teeth need removing?" stops being a general question and becomes a specific answer about your specific teeth. That clarity is the whole point of going in for the assessment.
What Each Path Actually Costs
Monitoring asymptomatic wisdom teeth costs essentially the price of a routine check-up with X-rays once a year or so, which is £50-£120 at most practices, or £20 at UrgentCare Dental for an emergency-pricing assessment if something changes. The ongoing cost of the watchful approach is genuinely modest.
Wisdom tooth extraction at UrgentCare Dental is £549 per tooth, or £695 with IV sedation if you'd prefer to be sedated for it (many patients do, especially for lower wisdom teeth). Across the UK generally, wisdom tooth removal runs £200-£600 per tooth privately, depending on complexity and practice.
Managing recurrent problems without extraction has a different cost pattern. Each flare-up is an emergency appointment (£20 at UrgentCare Dental) plus antibiotics (£9.90 in England). That's cheap per episode, but over two years, three or four episodes add up, and the real cost is in the pain, lost sleep, missed work, and disrupted life that each episode brings with it. For a tooth that's clearly going to keep causing trouble, the case for a single extraction over ongoing management is usually strong once you've been through it a couple of times.
The financial case is clearest when problems are recurring: one extraction cost versus the accumulating cost and misery of repeated emergencies. For asymptomatic teeth being monitored, the annual check-up cost is modest and the "wait and see" approach is genuinely the right call, not a cop-out.
Making the Decision Together
The decision about wisdom teeth removal should always be a conversation, not a pronouncement. A good dentist will explain their reasoning clearly and invite questions, and you should absolutely feel free to ask them.
If they're recommending removal: why specifically? What does the X-ray show that's driving this? What's the risk of leaving the tooth in? What's the expected complexity of the extraction, and what's the recovery like? If the recommendation is to monitor instead: what specifically are you watching for? How often should the next X-ray be, and what symptoms should prompt you to come back sooner? And if the recommendation is genuinely uncertain and sits in the grey zone: what factors are pointing toward removal, what factors are pointing toward leaving it, and what would change the balance either way?
At UrgentCare Dental, the wisdom tooth assessment includes an X-ray and a thorough conversation about whether removal is genuinely recommended, and if so, why, and if not, what we're watching for. The decision stays yours, informed by the clinical evidence and the dentist's experience, and you shouldn't feel rushed or pressured into anything.
Some wisdom teeth clearly need to come out. Some clearly don't. And for the ones in the middle, the question isn't a simple yes or no. It's "let's look at what your specific teeth are doing and work out what makes sense for you." That's the conversation worth having, and it's what a good assessment is actually for.
Need Emergency Dental Care?
Same-day appointments from just £20. Open 24 hours, 7 days a week.
